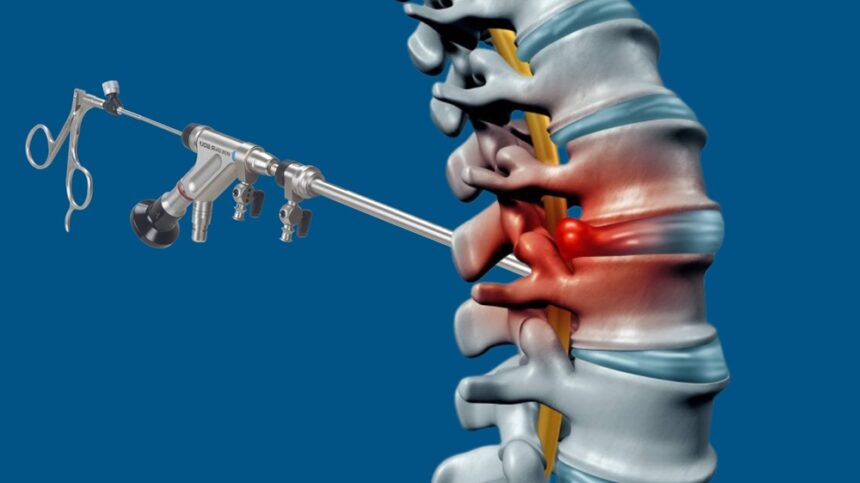
Frequently Asked Questions About Endoscopic Lumbar Surgery
This text has been prepared for general patient information within the scope of Prof. Dr. Semih Keskil’s academic areas of interest in spine surgery. There is no single, universally “best” method for every lumbar disc herniation patient. Diagnosis and treatment options are determined by evaluating the patient’s symptoms, physical examination findings, and MRI results together.
What does “endoscopic lumbar surgery” mean?
Answer: Methods referred to in daily practice as “totally boodless” or “fully closed” usually describe endoscopic or percutaneous (performed through a very small skin entry point) lumbar disc procedures. The goal is to remove the portion of the disc compressing the nerve (endoscopic discectomy) and, in suitable cases, to provide limited decompression of bone or ligament tissue causing nerve pressure.
The phrase “endoscopic surgical solution in lumbar disc disease” describes a family of surgical options; it is not suitable for every patient.
Can these operations be performed without general anesthesia?
Answer: Some endoscopic lumbar disc procedures can be performed with local anesthesia plus sedation; in other patients, general anesthesia may be preferred. The choice depends on the location of the herniation, the patient’s pain tolerance, coexisting diseases, and the extent of surgery.
Are endoscopic lumbar disc surgeries risky?
Answer: No surgical method has zero risk. However, low complication rates have been reported in the literature for endoscopic discectomy series. For example, in one meta-analysis, approximate rates were reported as:
• Dural tear: 1%
• Infection: 0.1%
• Temporary dysesthesia (sensory change): 1%
• Recurrence (re-herniation): 5.7%
“Open or closed?” Why are the terms confusing in lumbar disc surgery?
Answer:
• Microdiscectomy: A commonly used method performed under a microscope through a small skin incision.
• Endoscopic discectomy (often called fully closed or bloodless): Performed with an endoscope through a much smaller, needle-like entry point.
Which technique is chosen depends more on the type of herniation and the patient’s neurological findings than on the “open/closed” label.
What are the outcomes and reoperation rates after microdiscectomy?
Answer: In a systematic review, recurrence and reoperation rates after microdiscectomy varied among series; approximately 3–4% for recurrence and about 4–10% for reoperation have been reported. These rates may be influenced by factors such as age, disc characteristics, smoking, workload, and rehabilitation.
How is candidacy for endoscopic lumbar disc surgery evaluated?
Answer:
- Symptom–exam correlation: leg pain (sciatica) and signs of nerve compression
- MRI target confirmation: location of the disc fragment compressing the nerve
- Exclusion/management of urgent findings: progressive weakness, bladder–bowel control problems
- Comparison of options: endoscopic technique, microdiscectomy, and conservative follow-up
How is endoscopic lumbar disc surgery performed?
Answer:
- The patient is positioned appropriately on the operating table.
- In selected cases, local anesthesia and/or sedation may be used; in some patients, general anesthesia is preferred.
- Without a formal incision, an endoscope is inserted through a few-millimeter skin entry point.
- The herniated disc fragment compressing the nerve is removed.
- If necessary, limited bone or ligament tissue causing compression is trimmed.
- When the procedure is completed, the entry point closes on its own; sutures are usually not required.
In this respect, the method is one of the options described as an “endoscopic surgical solution” for lumbar disc disease. It is not a non-surgical treatment; it is still disc surgery. Even though it is performed through a needle-sized entry, the same essential steps as in open surgery may be required: bone trimming, removal of the disc fragment, opening and partial evacuation of the disc, and cauterization/repair of the treated area.
How long does recovery take after endoscopic lumbar disc surgery?
What is the hospital stay?
Answer: After endoscopic (fully closed) lumbar disc surgery, most patients can be discharged the same day or within a few hours. With other surgical methods such as microdiscectomy, hospital stay is often around one day.
What does “recovery” mean?
Answer: Recovery means:
• Closure of the surgical entry site
• Reduction of nerve-compression–related pain and symptoms
• Safe return to daily activities
Heavy lifting and strenuous work are not recommended before full recovery.
How long does it take to return to daily life?
Answer:
• Light daily activities: within a few days for most patients
• Desk work or light work: usually 1–2 weeks
• Heavy physical work: requires a controlled recovery period lasting weeks to months
Literature reports that approximately 70–80% of patients return to daily living activities within the first few weeks after endoscopic lumbar disc surgery.